Blog Details
Home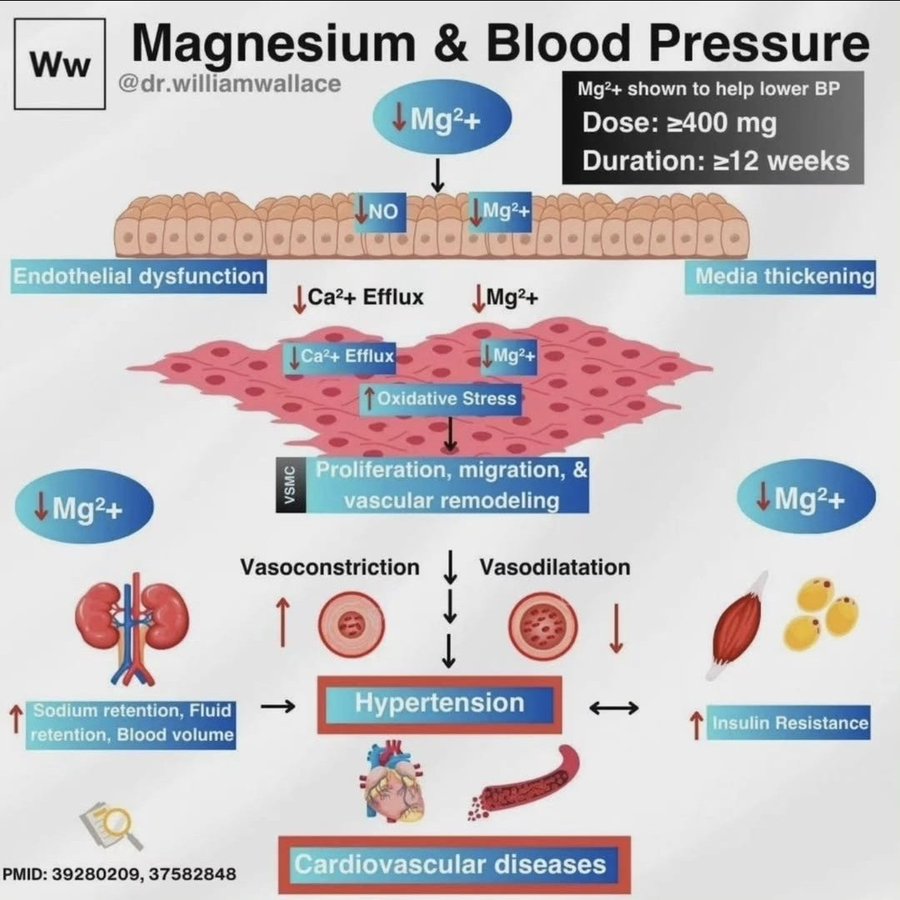
Magnesium Supplementation – Helps REDUCE Blood Pressure; Clinical Evidence
Systemic hypertension, also known as High Blood Pressure / BP – is a persistent elevation of the systemic arterial blood pressure (BP), and is a highly prevalent condition and a major independent risk factor of mortality and cardiovascular disease.
Preventing and treating hypertension has become a significant factor in decreasing the risk and burden of various diseases, thus reducing disease-related mortality. However, inadequate management of BP still remains one of the greatest individual risk factors of all-cause mortality globally, and each 10 mmHg rise in average systolic blood pressure (SBP) has been previously associated with an increase in cardiovascular disease (CVD) and chronic kidney disease risk by up to 16%.
Dietary and lifestyle modifications play major role in managing BP. Magnesium plays an important role in blood pressure regulation, as demonstrated by its influence on endothelial function, calcium efflux, and oxidative stress.
Magnesium deficiency can contribute to endothelial dysfunction, increased oxidative stress, and vascular remodeling, all of which exacerbate hypertension and cardiovascular disease risk.
Role of Magnesium in Blood Pressure Regulation
Magnesium is the fourth most common cation in the human body, and a deficient intake of magnesium has been associated with various diseases, including asthma, diabetes mellitus, hypertension, stroke, heart disease, hypertension, and even cancer.
Therefore, magnesium has been proposed as a treatment for hypertension. By inducing the formation of nitric oxide and prostacyclin, magnesium helps in modulating vasodilation, decreasing vascular tone and vascular reactivity.
Magnesium also possesses anti-inflammatory and as antioxidant properties and interacts with calcium, decreasing peripheral vascular resistance and thus decreasing blood pressure
Supplementation with magnesium has been shown to induce vasodilation, decrease vascular tone, and improve blood pressure outcomes.
Magnesium Helps Reduce BP – Clinical EVIDENCE
A recent umbrella meta-analyses (PMID: 39280209) found that magnesium doses ≥400 mg/day, administered for a duration of ≥12 weeks, can significantly reduce both systolic and diastolic blood pressure (SBP: -6.38 mmHg; DBP: -3.71 mmHg) - mostly in people with previous metabolic disorder (and also likely to have inadequate magnesium status before supplementing).
Mechanistically, magnesium influences nitric oxide production, prostaglandin synthesis, and calcium channel function, which collectively promote vasodilation and attenuate blood pressure increases.
Magnesium is one of the most common minerals in the human body, with 99% of it distributed intracellularly. The role of magnesium in reducing hypertension has been attributed to multiple mechanisms of action, including acting as a calcium channel blocker, competing with sodium binding sites on vascular smooth muscle cells, decreasing intracellular sodium and calcium, enhancing prostaglandin E, binding cooperatively with potassium, inducing vasodilation, improving endothelial dysfunction in diabetic and hypertensive patients.
Moreover, magnesium induces nitric oxide release from endothelial cells, which acts as vasoactive mediator and produces a synergistic effect with antihypertensive medications.
Magnesium Supplementation – Clinical Usage
In practice, ensuring sufficient magnesium intake may offer long-term cardiovascular benefits, especially when integrated into a broader strategy (as magnesium alone is not strong enough to function as a “monotherapy” for treating hypertension) targeting endothelial health, oxidative stress reduction, and vascular integrity.
A daily supplementation of good quality, chelated, highly bio-available Magnesium at 400 mg/day should be the starting point.
">
Systemic hypertension, also known as High Blood Pressure / BP – is a persistent elevation of the systemic arterial blood pressure (BP), and is a highly prevalent condition and a major independent risk factor of mortality and cardiovascular disease.
Preventing and treating hypertension has become a significant factor in decreasing the risk and burden of various diseases, thus reducing disease-related mortality. However, inadequate management of BP still remains one of the greatest individual risk factors of all-cause mortality globally, and each 10 mmHg rise in average systolic blood pressure (SBP) has been previously associated with an increase in cardiovascular disease (CVD) and chronic kidney disease risk by up to 16%.
Dietary and lifestyle modifications play major role in managing BP. Magnesium plays an important role in blood pressure regulation, as demonstrated by its influence on endothelial function, calcium efflux, and oxidative stress.
Magnesium deficiency can contribute to endothelial dysfunction, increased oxidative stress, and vascular remodeling, all of which exacerbate hypertension and cardiovascular disease risk.
Role of Magnesium in Blood Pressure Regulation
Magnesium is the fourth most common cation in the human body, and a deficient intake of magnesium has been associated with various diseases, including asthma, diabetes mellitus, hypertension, stroke, heart disease, hypertension, and even cancer.
Therefore, magnesium has been proposed as a treatment for hypertension. By inducing the formation of nitric oxide and prostacyclin, magnesium helps in modulating vasodilation, decreasing vascular tone and vascular reactivity.
Magnesium also possesses anti-inflammatory and as antioxidant properties and interacts with calcium, decreasing peripheral vascular resistance and thus decreasing blood pressure
Supplementation with magnesium has been shown to induce vasodilation, decrease vascular tone, and improve blood pressure outcomes.
Magnesium Helps Reduce BP – Clinical EVIDENCE
A recent umbrella meta-analyses (PMID: 39280209) found that magnesium doses ≥400 mg/day, administered for a duration of ≥12 weeks, can significantly reduce both systolic and diastolic blood pressure (SBP: -6.38 mmHg; DBP: -3.71 mmHg) - mostly in people with previous metabolic disorder (and also likely to have inadequate magnesium status before supplementing).
Mechanistically, magnesium influences nitric oxide production, prostaglandin synthesis, and calcium channel function, which collectively promote vasodilation and attenuate blood pressure increases.
Magnesium is one of the most common minerals in the human body, with 99% of it distributed intracellularly. The role of magnesium in reducing hypertension has been attributed to multiple mechanisms of action, including acting as a calcium channel blocker, competing with sodium binding sites on vascular smooth muscle cells, decreasing intracellular sodium and calcium, enhancing prostaglandin E, binding cooperatively with potassium, inducing vasodilation, improving endothelial dysfunction in diabetic and hypertensive patients.
Moreover, magnesium induces nitric oxide release from endothelial cells, which acts as vasoactive mediator and produces a synergistic effect with antihypertensive medications.
Magnesium Supplementation – Clinical Usage
In practice, ensuring sufficient magnesium intake may offer long-term cardiovascular benefits, especially when integrated into a broader strategy (as magnesium alone is not strong enough to function as a “monotherapy” for treating hypertension) targeting endothelial health, oxidative stress reduction, and vascular integrity.
A daily supplementation of good quality, chelated, highly bio-available Magnesium at 400 mg/day should be the starting point.
